Online first
About the Journal
Current issue
Archive
Publication Ethics
Anti-Plagiarism system
Instructions for Authors
Instructions for Reviewers
Editorial Office
Editorial Board
Contact
Reviewers
All Reviewers
2025
2024
2023
2022
2021
2020
2019
2018
2017
2016
General Data Protection Regulation (RODO)
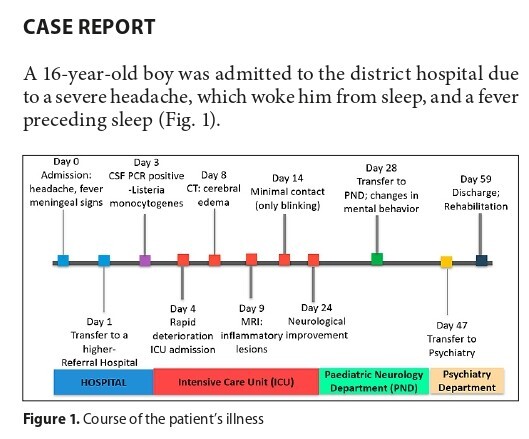
CASE REPORT
Complex neuropsychiatric disorders following Listeria monocytogenes encephalitis and meningitis in a 16-year-old
immunocompromised patient
1
Student Research Group, Department of Paediatric Neurology, Medical University, Lublin, Poland
2
Department of General Surgery, 1st Military Clinical Hospital with the Outpatient Clinic, Lublin, Poland
3
Department of Neonatology, Pathology and Neonatal Intensive Care, Stefan Cardinal Wyszyński District Specialist Hospital, Lublin, Poland
4
Department of Paediatric Neurology, Medical University, Lublin, Poland
Corresponding author
Natalia Biedroń
The Student Research Group, Department of Paediatric Neurology, Medical University, Lublin, Poland
The Student Research Group, Department of Paediatric Neurology, Medical University, Lublin, Poland
KEYWORDS
TOPICS
ABSTRACT
Introduction:
Listeriosis in immunocompetent patients usually presents as gastroenteritis with fever; however, it can occasionally lead to severe infections such as meningitis and sepsis. The case report concerns a boy with several autoimmune diseases on immunosuppressive therapy, who developed behavioural issues due to Listeria monocytogenes (LM) infection.
Case Report:
The patient was suspected of meningitis, and polymerase chain reaction testing of the cerebrospinal fluid revealed the presence of LM. The patient’s condition worsened, neurological symptoms increased, and the patient developed sepsis, requiring treatment in the Intensive Care Unit (ICU). After a monthly stay in the ICU, contact with the patient returned, but the infection caused severe behavioural changes. Autoimmune encephalitis was suspected and psychiatric treatment initiated.
Conclusions:
This case illustrates the broader issue of LM infection and emphasizes the need for special attention in the care of immunocompromised patients.
Listeriosis in immunocompetent patients usually presents as gastroenteritis with fever; however, it can occasionally lead to severe infections such as meningitis and sepsis. The case report concerns a boy with several autoimmune diseases on immunosuppressive therapy, who developed behavioural issues due to Listeria monocytogenes (LM) infection.
Case Report:
The patient was suspected of meningitis, and polymerase chain reaction testing of the cerebrospinal fluid revealed the presence of LM. The patient’s condition worsened, neurological symptoms increased, and the patient developed sepsis, requiring treatment in the Intensive Care Unit (ICU). After a monthly stay in the ICU, contact with the patient returned, but the infection caused severe behavioural changes. Autoimmune encephalitis was suspected and psychiatric treatment initiated.
Conclusions:
This case illustrates the broader issue of LM infection and emphasizes the need for special attention in the care of immunocompromised patients.
REFERENCES (24)
1.
Bento D, Bomar PA. Listeria Monocytogenes. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing, 2026.
2.
Xia X, Zhang L, Zheng H, et al. Clinical characteristics and prognosis of pediatric Listeria monocytogenes meningitis based on 10-year data from a large children’s hospital in China. Microbiol Spectr. 2024;12(3):e0324423. https://doi.org/10.1128/spectr....
3.
Liu YC, Liau SK, Hung CC, et al. Invasive Listeriosis in End-Stage Kidney Disease (ESKD) Patients Receiving Long-Term Dialysis: A 21-Year Case Series. Ther Clin Risk Manag. 2024;20:437–47. https://doi.org/10.2147/TCRM.S....
4.
European Food Safety Authority (EFSA), European Centre for Disease Prevention and Control (ECDC). The European Union One Health 2023 Zoonoses report. EFSA J. 2024;22(12):e9106. https://doi.org/10.2903/j.efsa....
5.
Lee JE, Cho WK, Nam CH, et al. A case of meningoencephalitis caused by Listeria monocytogenes in a healthy child. Korean J Pediatr. 2010;53(5):653. https://doi.org/10.3345/kjp.20....
6.
Castellazzi ML, Marchisio P, Bosis S. Listeria monocytogenes meningitis in immunocompetent and healthy children: a case report and a review of the literature. Ital J Pediatr. 2018;44(1):152. https://doi.org/10.1186/s13052....
7.
Villa A, Cour M, De Prost N, et al. Severe listeriosis in intensive care units: insights from a retrospective multicentric study. Crit Care. 2025;29(1):201. https://doi.org/10.1186/s13054....
8.
Żak-Gołąb A, Dąbrowski K, Hrycek A. Listeriosis of central nervous system in patients with ulcerative colitis – case study. Wiad Lek. 2017;70(3 pt 2):685–8.
9.
Trachuk P, Marin Saquicela T, Levi M, et al. Listeria brain abscess in a patient with autoimmune hepatitis. IDCases. 2019;17:e00569. https://doi.org/10.1016/j.idcr....
10.
Quereda JJ, Morón-García A, Palacios-Gorba C, et al. Pathogenicity and virulence of Listeria monocytogenes: A trip from environmental to medical microbiology. Virulence. 2021;12(1):2509–45. https://doi.org/10.1080/215055....
11.
Meireles D, Pombinho R, Cabanes D. Signals behind Listeria monocytogenes virulence mechanisms. Gut Microbes. 2024;16(1):2369564. https://doi.org/10.1080/194909....
12.
Ravindhiran R, Sivarajan K, Sekar JN, et al. Listeria monocytogenes an Emerging Pathogen: a Comprehensive Overview on Listeriosis, Virulence Determinants, Detection, and Anti-Listerial Interventions. Microb Ecol. 2023;86(4):2231–51. https://doi.org/10.1007/s00248....
13.
Olaimat AN, Al‐Holy MA, Shahbaz HM, et al. Emergence of Antibiotic Resistance in Listeria monocytogenes Isolated from Food Products: A Comprehensive Review. Compr Rev Food Sci Food Saf. 2018;17(5):1277–92. https://doi.org/10.1111/1541–4....
14.
Piekarska A, Panasiuk A, Stępień PM. Clinical practice guidelines for Clostridioides (Clostridium) difficile infection and fecal microbiota transplant protocol – recommendations of the Polish Society od Epidemiology and Infectious Diseases. Przegl Epidemiol. 2020;74(1):69–87. https://doi.org/10.32394/pe.74....
15.
Wall EC, Chan JM, Gil E, et al. Acute bacterial meningitis. Curr Opin Neurol. 2021;34(3):386–95. https://doi.org/10.1097/WCO.00....
16.
Watanabe A, Shiota T, Tsuji T. Cerebral edema during hepatic encephalopathy in fulminant hepatic failure. J Med. 1992;23(1):29–38.
17.
Cook AM, Morgan Jones G, Hawryluk GWJ, et al. Guidelines for the Acute Treatment of Cerebral Edema in Neurocritical Care Patients. Neurocrit Care. 2020;32(3):647–66. https://doi.org/10.1007/s12028....
18.
Kelley BP, Patel SC, Marin HL, et al. Autoimmune Encephalitis: Pathophysiology and Imaging Review of an Overlooked Diagnosis. AJNR Am J Neuroradiol. 2017;38(6):1070–8. https://doi.org/10.3174/ajnr.A....
19.
Cellucci T, Van Mater H, Graus F, et al. Clinical approach to the diagnosis of autoimmune encephalitis in the pediatric patient. Neurology(R) neuroimmunology & neuroinflammation. 2020;7(2). https://doi.org/10.1212/NXI.00....
20.
Song LF, Wang L, Tang ZH, et al. [Clinical features of autoimmune encephalitis secondary to epidemic encephalitis B in 5 children]. Zhongguo Dang Dai Er Ke Za Zhi. 2023;25(3):302–7. https://doi.org/10.7499/j.issn....
21.
Trewin BP, Freeman I, Ramanathan S, et al. Immunotherapy in autoimmune encephalitis. Curr Opin Neurol. 2022;35(3):399–414. https://doi.org/10.1097/WCO.00....
22.
Uy CE, Binks S, Irani SR. Autoimmune encephalitis: clinical spectrum and management. Pract Neurol. 2021;21(5):412–23. https://doi.org/10.1136/practn....
23.
Qiu X, Zhang H, Li D, et al. Analysis of Clinical Characteristics and Poor Prognostic Predictors in Patients With an Initial Diagnosis of Autoimmune Encephalitis. Front Immunol. 2019;10. https://doi.org/10.3389/fimmu.....
24.
Keeratiratwattana A, Saraya AW, Prakkamakul S. Computed tomography and magnetic resonance imaging findings in central nervous system listeriosis. Neuroradiology. 2024;66(5):717–27. https://doi.org/10.1007/s00234....
Share
RELATED ARTICLE
We process personal data collected when visiting the website. The function of obtaining information about users and their behavior is carried out by voluntarily entered information in forms and saving cookies in end devices. Data, including cookies, are used to provide services, improve the user experience and to analyze the traffic in accordance with the Privacy policy. Data are also collected and processed by Google Analytics tool (more).
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.