Online first
About the Journal
Current issue
Archive
Publication Ethics
Anti-Plagiarism system
Instructions for Authors
Instructions for Reviewers
Editorial Office
Editorial Board
Contact
Reviewers
All Reviewers
2025
2024
2023
2022
2021
2020
2019
2018
2017
2016
General Data Protection Regulation (RODO)
RESEARCH PAPER
A randomized controlled trial evaluating the efficacy and safety of a MYCOFUNGI CREAM in patients with skin mycoses
1
Antimicrobial and Biocontrol Agents Unit, Faculty of Science, LPMPS, University of Yaounde 1, Yaoundé, Cameroon
2
Drug Discovery and Development Research Unit, Laboratoire Roger Ducos, PO Box 20133 Yaounde, Cameroon
3
Department of Biochemistry, Faculty of Science, University of Bamenda, PO Box 39, Bambili, Cameroon
4
Elig-Essono Sub-divisional Medical Center, Elig-Essono, Yaounde, Cameroon
5
National Multi-sector Program to Combat Maternal, Newborn and Child Mortality (PLMI), Ministry of Public Health, Yaounde, Cameroon
6
Laboratory of Public Health Biotechnology, University of Yaoundé 1, Yaounde, Cameroon
Corresponding author
Patrick Valere Tsouh Fokou
Antimicrobial and Biocontrol Agents Unit, Faculty of Science, LPMPS, University of Yaounde 1, Yaoundé, Bambili, Cameroon
Antimicrobial and Biocontrol Agents Unit, Faculty of Science, LPMPS, University of Yaounde 1, Yaoundé, Bambili, Cameroon
J Pre Clin Clin Res. 2022;16(2):27-33
KEYWORDS
TOPICS
ABSTRACT
Introduction and objective:
Skin mycoses is a neglected condition with low quality of life and morbidity that primarily affects school-aged children in developing nations. Current treatment options have considerable limits, emphasizing the critical need for alternative therapies. The purpose of this clinical trial was to evaluate the potential benefit of Mycofungi cream in individuals with superficial fungal skin infection disorders.
Material and methods:
Patients with cutaneous mycoses ranging in age from 2–65 years were randomly assigned to either Mycofungi (Syzygium aromaticum (L.) Merr.) cream or Terbinafine creams. Within a four-week follow-up, the rates of cure or improvement were compared between the two groups. An incidental side-effect was also noted.
Results:
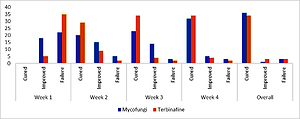
A total of 256 individuals with skin mycoses were preliminarily screened, and 80 eligible participants enrolled and randomly assigned to the Mycofungi (n=40) or Terbinafine (n=40) groups. Overall, 92.5% (37/40) of patients with cutaneous mycoses were asymptomatic or had improved condition following Mycofungi application at the final follow-up appointment. After four weeks of treatment, the clinical cure rate was high and nearly identical in the two groups: 80% in the Mycofungi group and 85% in the Terbinafine group. Both terbinafine and mycofungy were well tolerated.
Conclusions:
The efficacy of Mycofungi cream (S. aromaticum) in treating or reducing the severity of skin mycoses was proven in this clinical trial. Nonetheless, additional detailed experiments are needed to reach a conclusion on the efficacy of Mycofungi.
Skin mycoses is a neglected condition with low quality of life and morbidity that primarily affects school-aged children in developing nations. Current treatment options have considerable limits, emphasizing the critical need for alternative therapies. The purpose of this clinical trial was to evaluate the potential benefit of Mycofungi cream in individuals with superficial fungal skin infection disorders.
Material and methods:
Patients with cutaneous mycoses ranging in age from 2–65 years were randomly assigned to either Mycofungi (Syzygium aromaticum (L.) Merr.) cream or Terbinafine creams. Within a four-week follow-up, the rates of cure or improvement were compared between the two groups. An incidental side-effect was also noted.
Results:
A total of 256 individuals with skin mycoses were preliminarily screened, and 80 eligible participants enrolled and randomly assigned to the Mycofungi (n=40) or Terbinafine (n=40) groups. Overall, 92.5% (37/40) of patients with cutaneous mycoses were asymptomatic or had improved condition following Mycofungi application at the final follow-up appointment. After four weeks of treatment, the clinical cure rate was high and nearly identical in the two groups: 80% in the Mycofungi group and 85% in the Terbinafine group. Both terbinafine and mycofungy were well tolerated.
Conclusions:
The efficacy of Mycofungi cream (S. aromaticum) in treating or reducing the severity of skin mycoses was proven in this clinical trial. Nonetheless, additional detailed experiments are needed to reach a conclusion on the efficacy of Mycofungi.
ACKNOWLEDGEMENTS
The authors thank all participants for their cooperation. We also thank Dr Bita Gertrude, the then Director of the Elig-Essono Sub-divisional Medical Center, Yaounde, Cameroon, for granting authorization to conduct the study.
Youmsi Fokouo RD, Tsouh Fokou PV, Choakem G, Nhanag S, Majoumouo MS, Tamko JL, Chedjou JP, Kuete G, Fon Mbacham W, Fekam Boyom
F. A randomized controlled trial evaluating the efficacy and safety of a MYCOFUNGI CREAM in patients with skin mycoses. J Pre-Clin Clin Res.
2022; 16(2): 27–33. doi: 10.2644/jpccr/150030
REFERENCES (33)
1.
WHO. Recognizing neglected tropical diseases through changes on the skin A training guide for front-line health workers. Control of Neglected Tropical Diseases. WHO/HTM/NTD/2018.03 ed. Geneva, 2018, p. 48.
2.
Hay RJ, Asiedu K. Skin-Related Neglected Tropical Diseases (Skin NTDs) – a new challenge. Trop Med Infect Dis. 2018; 4(1): 4.
3.
de Macedo PM, Freitas DFS. Superficial Infections of the skin and nails. In: Zaragoza O, Casadevall A, editors. Encyclopedia of Mycology. Ed. 1. Elsevier; 2021. p. 707–718.
4.
Kühbacher A, Burger-Kentischer A, Rupp S. Interaction of Candida Species with the skin. Microorganisms. 2017; 5(2): 32.
5.
Prawer S, Prawer S, Bershow A. Superficial Fungal Infections. In: Soutor C, Hordinsky MK, editors. Clinical Dermatology. Ed. 1. McGraw Hill; 2013. p. 71.
6.
Kwon-Chung KJ, Bennett JE. Medical mycology. Rev Inst Med Trop Sao Paulo. 1992; 34(6): 504–504.
7.
Capoci IRG, Sakita KM, Faria DR, et al. Two New 1,3,4-Oxadiazoles with effective antifungal activity against Candida albicans. Front Microbiol. 2019; 10: 2130–2130.
8.
Saunte DML, Gaitanis G, Hay RJ. Malassezia-associated skin diseases, the use of diagnostics and treatment. Front Cell Infect Microbiol. 2020; 10: 112–112.
9.
Vlachos C, Henning MAS, Gaitanis G, et al. Critical synthesis of available data in Malassezia folliculitis and a systematic review of treatments. J Eur Acad Dermatol Venereol. 2020; 34(8): 1672–1683.
10.
Thayikkannu AB, Kindo AJ, Veeraraghavan M. Malassezia-Can it be Ignored? Indian J Dermatol. 2015; 60(4): 332–339.
11.
Karray M, McKinney WP. Tinea Versicolor. [Updated 2021 Aug 11]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan-. Available from: https://www.ncbi.nlm.nih.gov/b....
12.
Coulibaly O, L’Ollivier C, Piarroux R, et al. Epidemiology of human dermatophytoses in Africa. Med Mycol. 2018; 56(2): 145–161.
13.
Abd Elmegeed ASM, Ouf SA, Moussa TAA, et al. Dermatophytes and other associated fungi in patients attending to some hospitals in Egypt. Braz J Microbiol. 2015; 46(3): 799–805.
14.
Didehdar M, Shokohi T, Khansarinejad B, et al. Characterization of clinically important dermatophytes in North of Iran using PCR-RFLP on ITS region. J Mycol Med. 2016; 26(4): 345–350.
15.
Ganne A. Les mycoses superficielles a l’officine: description clinique, traitement et prevention. Limoges: Universite de Limoges; 2012.
16.
Gong Y, Liu W, Huang X, et al. Antifungal activity and potential mechanism of n-butylphthalide alone and in combination with fluconazole against Candida albicans. Front Microbiol. 2019; 10(1461): 1461.
17.
Verma S, Heffernan MP. Superficial fungal infections: dermatophytosis, onychomycosis, tinea nigra, piedra. In: Wolff K, Goldsmith LA, Katz SI, Gilchrest BA, Paller AS, Leffell DJ, editors. Fitzpatrick’s dermatology in general medicine. Ed. 7. McGraw-Hill; 2008. p. 1807–1821.
18.
Hay RJ, Ashbee HR. Superficial mycoses. In: Burns T BS, Cox N, Griffiths C, editor. Rook’s Textbook of Dermatology. Ed. 8 Wiley-Blackwell; 2010. p. 36.5–36.68.
19.
Dias MF, Bernardes-Filho F, Quaresma-Santos MV, et al. Treatment of superficial mycoses: review. Part II. An Bras Dermatol. 2013; 88(6): 937–944.
20.
McKeny PT, Nessel TA, Zito PM. Antifungal Antibiotics. [Updated 2021 Nov 15]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan-. Available from: https://www.ncbi.nlm.nih.gov/b....
21.
Pfaller MA, Diekema DJ. Epidemiology of invasive mycoses in North America. Crit Rev Microbiol. 2010; 36(1): 1–53.
22.
da Matta DA, Souza ACR, Colombo AL. Revisiting Species Distribution and Antifungal Susceptibility of Candida Bloodstream Isolates from Latin American Medical Centers. J Fungi (Basel). 2017; 3(2): 24.
23.
Sanguinetti M, Posteraro B, Lass-Flörl C. Antifungal drug resistance among Candida species: mechanisms and clinical impact. Mycoses. 2015; 58: 2–13.
24.
Vandeputte P, Ferrari S, Coste AT. Antifungal resistance and new strategies to control fungal infections. Int J Microbiol. 2012; 2012: 713687.
25.
Al-Bader SM, Moqbel FS. Effect of Selected Plant Extracts on Malssezia Furfur in Culture. Eurasian J Sci Eng. 2017;3 (special):43.
26.
Fokouo RDY, Fokou PVT, Mbouna CDJ, et al. Antidermatophyte activity of Syzygium aromaticum, Petroselinum crispum, and Tetrapleura tetraptera. Biomed Biotechnol Res J. 2020; 4(1): 55.
27.
Pinto E, Vale-Silva L, Cavaleiro C, et al. Antifungal activity of the clove essential oil from Syzygium aromaticum on Candida, Aspergillus and dermatophyte species. J Med Microbiol. 2009; 58(Pt 11): 1454–1462.
28.
Rana IS, Rana AS, Rajak RC. Evaluation of antifungal activity in essential oil of the Syzygium aromaticum (L.) by extraction, purification and analysis of its main component eugenol. Braz J Microbiol. 2011; 42: 1269–1277.
29.
Yassin MT, Mostafa AA-F, Al-Askar AA. In vitro anticandidal potency of Syzygium aromaticum (clove) extracts against vaginal candidiasis. BMC Complement Med Ther. 2020; 20(1): 25.
30.
Fokouo RDY, Fokou PVT, Mbouna CDJ, et al. Formulation and evaluation of safety and antifungal efficacy of Syzigium aromaticum-base cream on Guinea pigs infected with Trichophyton mentagrophytes. Pharmacog J. 2020; 12(2).
31.
Abhinav C, Mahajan VK, Mehta KS, et al. Allergic contact dermatitis due to clotrimazole with cross-reaction to miconazole. Indian J Dermatol Venereol Leprol. 2015; 81(1): 80–82.
32.
Panahi Y, Akhavan A, Sahebkar A, et al. Investigation of the effectiveness of Syzygium aromaticum, Lavandula angustifolia and Geranium robertianum essential oils in the treatment of acute external otitis: A comparative trial with ciprofloxacin. J Microbiol Immunol Infect. 2014; 47(3): 211–216.
33.
Kubatka P, Uramova S, Kello M, et al. Antineoplastic effects of clove buds (Syzygium aromaticum L.) in the model of breast carcinoma. J Cell Mol Med. 2017; 21(11): 2837–2851.
We process personal data collected when visiting the website. The function of obtaining information about users and their behavior is carried out by voluntarily entered information in forms and saving cookies in end devices. Data, including cookies, are used to provide services, improve the user experience and to analyze the traffic in accordance with the Privacy policy. Data are also collected and processed by Google Analytics tool (more).
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.