Online first
About the Journal
Current issue
Archive
Publication Ethics
Anti-Plagiarism system
Instructions for Authors
Instructions for Reviewers
Editorial Office
Editorial Board
Contact
Reviewers
All Reviewers
2025
2024
2023
2022
2021
2020
2019
2018
2017
2016
General Data Protection Regulation (RODO)
RESEARCH PAPER
The prevalence and risk factors for latent Mycobacterium tuberculosis infection in patients with chronic kidney disease
1
Chair and Department of Nephrology, Medical University, Lublin, Poland
2
Chair and Department of Medical Microbiology, Medical University, Lublin, Poland
Corresponding author
Anna Steć
Chair and Department of Nephrology, Medical University, Lublin, Dr K. Jaczewskiego 8, 20-954 Lublin, Poland
Chair and Department of Nephrology, Medical University, Lublin, Dr K. Jaczewskiego 8, 20-954 Lublin, Poland
J Pre Clin Clin Res. 2023;17(1):1-4
KEYWORDS
TOPICS
ABSTRACT
Introduction and objective:
Active tuberculosis (TB), which develops mostly in the mechanism of latent tuberculosis infection (LTBI) activation, is a difficult and important problem among patients with chronic kidney disease (CKD). The aim of the study was to determine the prevalence of LTBI and associated risk factors in CKD patients, both undergoing dialysis and in the pre-dialysis stage.
Material and methods:
The study comprised 482 subjects aged 19–98, including 294 haemodialysis, 50 peritoneal dialysis and 32 pre-dialysis patients, as well as 106 healthy controls. In order to determine LTBI, QuantiFERON Gold In-Tube Test (QFT-GIT, Cellestis Ltd, Australia) was used.
Results:
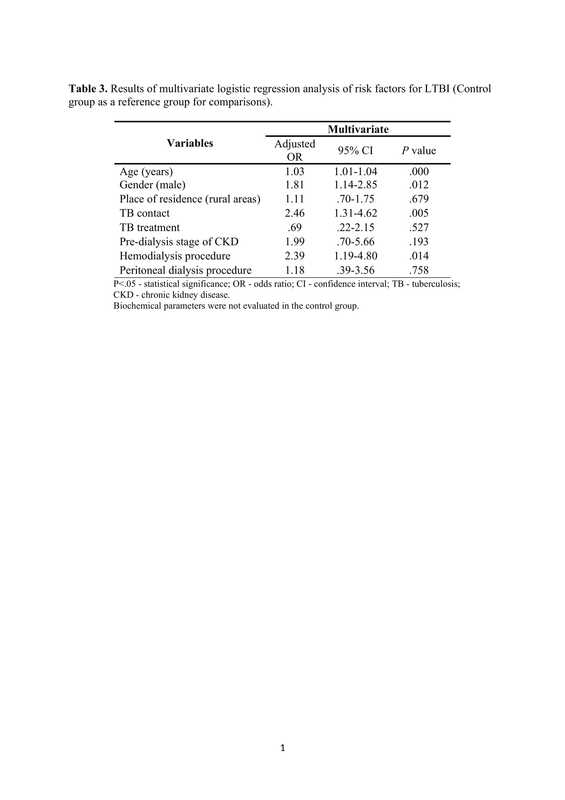
Positive QFT-GIT test was obtained in 32% haemodialysis, 28.1% pre-dialysis, 12% peritoneal dialysis patients, and in 11.3% controls. By univariate logistic regression analysis, predictors of LTBI were: active smoking (OR=1.34), coronary artery disease (OR=1.32), age (OR=1.04), male gender (OR=1.42), platelet count (OR=1.00), and duration of dialysis (OR=.95). By multivariate logistic regression, independent predictors of LTBI were: age (OR=1.02), male (OR=1.81), haemodialysis procedure (OR=2.39), TB contact (OR=2.46) and platelet count (OR=.99).
Conclusions:
The obtained results revealed a high prevalence of LTBI in CKD patients. Established risk factors, especially those described for the first time, such as platelet count and coronary artery disease, provided clinical support in TB diagnosis. Since a high LTBI rate in CKD patients was observed, wide use of the QFT-GIT test is recommend to control TB in this population.
Active tuberculosis (TB), which develops mostly in the mechanism of latent tuberculosis infection (LTBI) activation, is a difficult and important problem among patients with chronic kidney disease (CKD). The aim of the study was to determine the prevalence of LTBI and associated risk factors in CKD patients, both undergoing dialysis and in the pre-dialysis stage.
Material and methods:
The study comprised 482 subjects aged 19–98, including 294 haemodialysis, 50 peritoneal dialysis and 32 pre-dialysis patients, as well as 106 healthy controls. In order to determine LTBI, QuantiFERON Gold In-Tube Test (QFT-GIT, Cellestis Ltd, Australia) was used.
Results:
Positive QFT-GIT test was obtained in 32% haemodialysis, 28.1% pre-dialysis, 12% peritoneal dialysis patients, and in 11.3% controls. By univariate logistic regression analysis, predictors of LTBI were: active smoking (OR=1.34), coronary artery disease (OR=1.32), age (OR=1.04), male gender (OR=1.42), platelet count (OR=1.00), and duration of dialysis (OR=.95). By multivariate logistic regression, independent predictors of LTBI were: age (OR=1.02), male (OR=1.81), haemodialysis procedure (OR=2.39), TB contact (OR=2.46) and platelet count (OR=.99).
Conclusions:
The obtained results revealed a high prevalence of LTBI in CKD patients. Established risk factors, especially those described for the first time, such as platelet count and coronary artery disease, provided clinical support in TB diagnosis. Since a high LTBI rate in CKD patients was observed, wide use of the QFT-GIT test is recommend to control TB in this population.
Steć A, Magryś A, Załuska W. The prevalence and risk factors for latent Mycobacterium tuberculosis infection in patients with chronic kidney
disease. J Pre-Clin Clin Res. 2023; 17(1): 1–4. doi: 10.26444/jpccr/160170
REFERENCES (23)
1.
Shu CC, Hsu CL, Wei YF, et al. Risk of Tuberculosis Among Patients on Dialysis: The Predictive Value of Serial Interferon-Gamma Release Assay. Medicine. 2016;95(22):e3813. https://doi.org/10.1097/MD.000....
2.
Romanowski K, Clark EG, Levin A, et al. Tuberculosis and chronic kidney disease: an emerging global syndemic. Kidney Int. 2016;90(1):34–40. https://doi.org/10.1016/j.kint....
3.
Okada RC, Barry PM, Skarbinski J, et al. Epidemiology, detection, and management of tuberculosis among end-stage renal disease patients. Infect Control Hosp Epidemiol. 2018;39(11):1367–1374. https://doi.org/10.1017/ice.20....
4.
Vikrant S. Clinical profile of tuberculosis in patients with chronic kidney disease: A report from an endemic Country. Saudi J Kidney Dis Transpl. 2019;30(2):470–477. https://doi.org/10.4103/1319-2....
5.
Latent TB infection: updated and consolidated guidelines for programmatic management.
7.
Campbell JR, Johnston JC, Ronald LA, et al. Screening for latent tuberculosis infection in migrants with CKD: a cost-effectiveness analysis. Am J Kidney Dis. 2019;73:39–50. https://doi.org/10.1053/j.ajkd....
8.
Rogerson TE, Chen S, Kok J, et al. Tests for latent tuberculosis in people with ESRD: a systematic review. Am J Kidney Dis. 2013;61:33–43. https://doi.org/10.1053/j.ajkd....
9.
Shu CC, Wu VC, Yang FJ, et al. Predictors and prevalence of latent tuberculosis infection in patients receiving long-term hemodialysis and peritoneal dialysis. PLoS One. 2012;7(8):e42592. https://doi.org/10.1371/journa....
10.
Shu CC, Hsu CL, Lee CY, et al. Comparison of the Prevalence of Latent Tuberculosis Infection among Non-Dialysis Patients with Severe Chronic Kidney Disease, Patients Receiving Dialysis, and the Dialysis-Unit Staff: A Cross-Sectional Study. PLoS One. 2015; 28;10(4):e012410410. https://doi.org/10.1371/journa....
11.
Moran E, Baharani J, Dedicoat M, et al. Risk factors associated with the development of active tuberculosis among patients with advanced chronic kidney disease. Journal of Infection. 2018;77(4); 291–295. https://doi.org/10.1016/j.jinf....
12.
Basham CA, Smith SJ, Romanowski K, et al. Cardiovascular morbidity and mortality among persons diagnosed with tuberculosis: A systematic review and meta-analysis. PLoS ONE. 2020;15(7):e0235821. https://doi.org/10.1371/journa....
13.
Chung WS, Lin CL, Hung CT, et al. Tuberculosis increases the subsequent risk of acute coronary syndrome: a nationwide population-based cohort study. Int J Tuberc Lung Dis. 2014;18(1):79–83. https://doi.org/10.5588/ijtld.....
14.
Huaman MA, Ticona E, Miranda G, et al. The Relationship Between Latent Tuberculosis Infection and Acute Myocardial Infarction. Clin Infect Dis. 2018;66:886–892. https://doi.org/10.1093/cid/ci....
15.
Fioranelli M, Bottaccioli AG, Bottaccioli F, et al. Stress and Inflammation in Coronary Artery Disease: A Review Psychoneuroendocrineimmunology-Based. Front Immunol. 2018;9:2031. https://doi.org/10.3389/fimmu.....
16.
Rota S, Rota S. Mycobacterium tuberculosis complex in atherosclerosis. Review. Acta Med Okayama. 2005;59:247–251. https://doi.org/10.18926/AMO/3....
17.
Rota S, Tuncer S, Rota S, Kanat O. Mycobacterium tuberculosis complex DNA does not exist in atheromatous plaques. New Microbiol. 2005;28:165–169.
18.
Huaman M, Henson D, Ticona E, et al. Tuberculosis and Cardiovascular Disease: Linking the Epidemics. Tropical Diseases, Travel Medicine and Vaccines. 2015;1:10 https://doi.org/10.1186/s40794....
19.
Zhang Y, Xiong Q, Hu X, et al. A novel atherogenic epitope from Mycobacterium tuberculosis heat shock protein 65 enhances atherosclerosis in rabbit and LDL receptor-deficient mice. Heart Vessels. 2012;27:411–418. https://doi.org/10.1007/s00380....
20.
Grundtman C, Jakic B, Buszko M, Onestingel E, et al. Mycobacterial heat shock protein 65 (mbHSP65)-induced atherosclerosis: Preventive oral tolerization and definition of atheroprotective and atherogenic mbHSP65 peptides. Atherosclerosis. 2015;242(1):303–10. https://doi.org/10.1016/j.athe....
21.
Auguste P, Tsertsvadze A, Pink J, et al. Comparing interferon-gamma release assays with tuberculin skin test for identifying latent tuberculosis infection that progresses to active tuberculosis: systematic review and meta-analysis. BMC Infect Dis. 2017;17(1):200. https://doi.org/10.1186/s12879....
22.
Myall K, Milburn HJ. An update on the management of latent tuberculosis infection and active disease in patients with chronic kidney disease. Pol Arch Intern Med. 2017;127(10): 681–686. https://doi.org/10.20452/pamw.....
23.
Augustynowicz-Kopec E, Demkow U, Grzelewska-Rzymowska I, et al. Guidelines of Polish Respiratory Society concerning diagnosis, treatment and prevention of tuberculosis in adults and in children. Pneumonol Alergol Pol. 2013;81:323–379.
We process personal data collected when visiting the website. The function of obtaining information about users and their behavior is carried out by voluntarily entered information in forms and saving cookies in end devices. Data, including cookies, are used to provide services, improve the user experience and to analyze the traffic in accordance with the Privacy policy. Data are also collected and processed by Google Analytics tool (more).
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.